
Images and text Genevieve Carbonatto
A 55 year old man with bilateral renal transplants and diabetes presents to the Emergency department with a 6 day history of right upper quadrant pain and severe back pain, fever, diarrhea, nausea and vomiting.
On examination his HR is 95/min. He has a systolic BP of 97, and he is saturating 95% on room air. He is afebrile. He is very lethargic, finds it difficult to answer questions and appears jaundiced. He is tender in the RIF and less so in the RUQ. He has a distended but not peritonitic abdomen. These are his bloods : Creatinine 518umol/l from a baseline of 97 umol/l, glucose 27.1mmol/l, total bilirubin 80 umol/l with elevated LFT, amylase 122 U/l, WCC 25.3, CRP 482 mg/l.
The concern is that he has complicated cholecystitis and you are asked to do a Point of Care Ultrasound to look at his gallbladder. The gall bladder appears normal, the CBD is not dilated, the liver has normal echogenicity. You notice the small bowel has absent peristalsis. With your probe you examine the abdomen and you notice that the area of maximum tenderness is in the RIF over the right transplant kidney. This is his right transplant kidney.
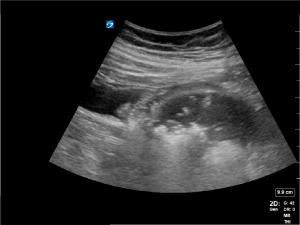

This is an emphysematous kidney. Notice the coarse echogenic foci associated with “dirty shadowing”. This is gas within the renal parenchyma.


The left transplant kidney looks normal
A CT scan showed extensive amount of gas in the renal parenchyma confirming the diagnosis of emphysematous kidney.

His had a predominant growth of E coli in his urine and E coli in his blood cultures. He went emergently to theatre for a right renal transplant nephrectomy, was started on tazosin and recommenced haemodylsis in ICU.
Discussion
Ultrasound features of a normal kidney are
- Hyperechoic renal capsule
- Isoechoic or hypoechoic parcenchyma (cortex and meduclla) compared with the normal liver or spleen
- The cortex and medulla usually have the same echogenicity. The medulla may be slightly darker
- Hyperechoic renal sinus

Normal kidney
Emphysematous pylenonephritis (EPN) is a fulminant, life threatening, necrotising infection of the renal parenchyma that is associated with gas formation in the kidney or in the perinephric space. EPN should be differentiated from emphysematous pyelitis that is characterized by gas in the pelvicaliceal system only. Emphysematous pyelitis is a benign disease and a complete recovery can be achieved with medical treatment. By contrast, EPN has a high mortality. (2)
Characteristics of EPN:
- Usually associated with diabetes or immunosuppression (TB, AIDS, alocoholism, renal transplant)
- In diabetic patients, EPN tends to occur in nonobstructed kidneys
- In non diabetic patients, EPN tends to occur in obstructed kidneys
- Higher incidence in women
- Left kidney affected more than right kidney
- Bilateral disease occurs in 5 -10% of patients
- E coli is the most common organism isolated
- Klebsiella, Proteus, pseudomonas also implicated
Diagnosis
CT is the best imaging modality. The location and extent of gas in the parenchyma or perinephric space is easily identified. EPN can be classified into 4 classes according to CT findings (Huang and Tseng classification)
- Class 1: Gas in the collecting system only.
- Class 2: Parenchymal gas only.
- Class 3a: Extension of gas into perinephric space.
- Class 3b: Extension of gas into paranephric space.
- Class 4: EPN presents in one or both kidneys.
Wan, et al, on the other hand, have classified EPN as types I and II based on CT findings.
- Type I is characterized by renal necrosis together with the presence of gas but without fluid.
- Type II is characterized by parenchymal gas associated with fluid in the renal parenchyma, perinephric space or the collecting system.
Ultrasound is not the preferred imaging modality. Intrarenal gas causes high-amplitude echoes within the renal sinus/renal parenchyma associated with dirty acoustic shadowing, and ring-down artifacts may result from air bubbles trapped in fluid. Gas will obscure deeper structures. It may obscure the kidney completely or prompt the erroneous interpretation of renal calculi or bowel gas.
Treatment is emergency nephrectomy.
Teaching point: The brief in this case was to scan for biliary pathology. The outcome was the identification of life threatening renal pathology. The importance of Point of Care Ultrasound in the workup of a patient presenting to the Emergency Department cannot be overestimated in the context of improving diagnostic ability.
References:
- Spectrum of gas within the kidney: Emphysematous pyelonephritis and emphysematous pyelitis
Author links open overlay panelG.V.EvanoffM.D.C.S.ThompsonM.D.R.FoleyM.D.E.J.WeinmanM.D
The American journal of medicine Volume 83, Issue 1, July 1987, Pages 149-154 - Emphysematous Pyelonephritis in a Transplant Kidney
M. Salehipour, J. Roozbeh, A. R. Rasekhi, M. A. Afrasiabi, H. Rezaee, K. Izadpanah, and S. A. Malek-Hosseini Int J Organ Transplant Med. 2010; 1(1): 49–51. - Radiopaedia
- Medscape : Emphysematous pyelonephritis




