
Ultrasound images Genevieve Carbonatto and Tina Cullen text Genevieve Carbonatto
A 35 year old man presents to the Emergency Department with acute onset right flank pain. He has been having “niggles” of pain in the last week but suddenly at work he develops severe pain. He has microscopic haematuria on a urinary dip stick. You think this is renal colic. He is given analgesia, opiates and nonsteroidal antiinflammatories and his pain settles. You decide to do an ultrasound while he is pain free.
The image on the left is of his right kidney in longitudinal section (13.7 cm in length) . The image on the right is a longitudinal image of his left kidney (12.7 cm in length).


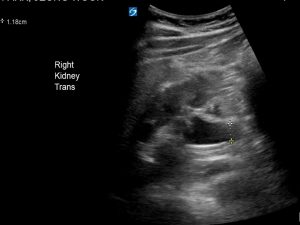
Below is the transverse view of his right kidney. Note the calyceal dilatation and proximal ureteric dilatation (1.18cm) of his right kidney indicating mild hydronephrosis.

Below is his bladder in transverse. A small stone is visible at the VUJ. Note that it does cast an acoustic shadow.


A larger stone, >3- 5 mm will cast an acoustic shadow as seen in this different case below.


Using Doppler, a reduced jet is visible in our patient on the right compared to the left indicating partial obstruction of the right ureter.
The right ureter is also visible and dilated indicating mild hydroureter.


What should you be looking for on ultrasound when examining the renal system in the context of renal colic?
- Stone: The sensitivity of detection is variable according to different studies, ranging from 24% to 96% depending on operator experience . Detection is size dependent. Stones <3mm have a high non detection rate (70% in one study) (1) Some features of stones include,
- They appear as hyperechoic foci with posterior shadowing
- If <5mm may not be seen and posterior shadowing may not be present
- Unable to detect in mid-ureter
- Twinkling artifact increases the sensitivity of detection from 27.6 % to 86% in one study (11) with a sensitivity of 90% and a specificity of 100% in another.(10)
2. Hydronephrosis
- If there is complete or near complete obstruction.
- May not be present in the early phase of obstruction (not enough time to develop)
- May not be present in dehydrated patients
- Minimal if stones are small
3. Absent, asymmetric +/- or reduced ureteric jet
Discussion
Some facts about renal colic
- Prevalence ranges between 2 and 8%.
- Peak presentation for men age 40 -50, for women late 20’s
- 80% contain calcium crystals
- Risk factors for stone formation include warm climates (due to dehydration), patients producing less than 1 L of urine a day, obesity, family history, any abnormality of the renal tract medical disorders (hyperparathyroidism, chronic diarrhoeal disorders, myeloprolipherative disorders and renal tubular acidosis)
- 90% of stones will pass spontaneously.
- 50% of patients with stones will have a recurrence within 10 years.
Urinalysis
- 90% of patients with renal colic will have microscopic haematuria
- 40% of patients with flank pain and haematuria do not have renal colic. Consider other diagnoses (UTI, pyelonephritis, AAA, diverticulitis, pneumonia, small bowel obstruction, cholecystitis, pelvic inflammatory disease)
Location of stones
- Pelvi ureteric junction (10%)
- Proximal ureter (23%)
- Mid ureter where the ureter crosses the iliac vessels (2%)
- Vesico ureteric junction (60%)
Which stones are likely to pass?
- overall 90% of stones will pass spontaneously
- 70% of stones < 5 mm will pass spontaneously
- 47% of stones between 5-10 mm will pass spontaneously
- the smaller the stone the faster the passage over time. Larger stones may take up to 3 weeks to pass.
Who needs imaging in the Emergency Department?
- First episode of renal colic
- Clinical symptoms not improving with analgesia
- Abnormal renal function or presence of inflammatory markers
- Representation with pain within a few days of initial episode
- Renal colic + sepsis
- Diagnostic uncertainty
Who needs urgent surgical intervention?
- Presence of an obstructive infected kidney
- Obstruction of a solitary kidney
- Bilateral obstruction
- Uncontrolled pain
There are numerous advantages of using ultrasound as a first line imaging modality in patients with renal colic. In a study comparing emergency department point of care ultrasound with CT, initial ultrasonography was associated with lower cumulative radiation exposure that initial CT without significant differences in high- risk diagnosis with complications, serious adverse events, pain scores, return emergency department visits or hospitalisations. (8) Simple uncomplicated renal colic can be treated by “waiting and seeing” while doing a point of care ultrasound to look directly for stones or to look for indirect signs of stones such as hydronephrosis. First presentation of renal colic warrants an initial low dose CT KUB as do more complicated cases such as recurrent presentations, renal colic without haematuria, diabetic patients, single kidney, renal transplant, renal impaired patients or patients presenting with a diagnostic dilemma. Below are some advantages and disadvantages of using ultrasound vs CT in the emergency department.
Ultrasound
+ves
- reproducible
- non invasive
- non expensive
- no ionising radiation
- can identify stones especially if > 5mm in the kidney, VUJ or bladder.
- may show hydronephrosis (indirect sign)
-ves
- if the examination is normal it does not exclude renal colic
- operator dependent
CT
+ves
- Excellent accuracy in detecting location and size of stones (sensitivity 95-97%, specificity 96 -100%) (4)
- Able to detect alternative causes of pain- 10% (AAA, appendicitis, cholecystitis)
- Possible to use low dose radiation CT imaging but often not used (9)
-ve
- Cumulative exposure of radiation as patients tend to have repeated CTs when presenting to the Emergency Department with flank pain and haematuria.
- cost
Teaching point: Consider each patient with renal colic and decide on the best imaging modality. If you decide to do a CT scan then ask for a low dose CT scan. If the patient has had previous CTs and is uncomplicated in their presentation then focussed point of care ultrasound is sufficient as an initial investigation in the emergency department . Remember that non low dose CT scans are associated with a not insignificant risk of cancer in young patients. Ultrasound should be the initial investigation in all young women and in children.
References
- Insights imaging : 2015 Aug; 6(4): 441–447. Imaging patients with renal colic—consider ultrasound first Carlos Nicolau,corresponding author Michel Claudon, Lorenzo E. Derchi, E. Jane Adam, Michael Bachmann Nielsen, Gerhard Mostbeck, Catherine M. Owens, Christiane Nyhsen, and Spyros Yarmenitis.
- Nephron Clin Practice: 2010;116(3):c159-71. An update and practical guide to renal stone management. Johri N1, Cooper B, Robertson W, Choong S, Rickards D, Unwin R.
- J Emerg Med. 2007;33:161–168.2006.12.035.Broder J, Bowen J, Lohr J, et al. Cumulative CT exposures in emergency department patients evaluated for suspected renal colic.
- Insights Imaging. 2014;5:217–230. McLaughlin PD, Murphy KP, Hayes SA, et al. Non-contrast CT at comparable dose to an abdominal radiograph in patients with acute renal colic; impact of iterative reconstruction on image quality and diagnostic performance.
- Br J Radiol. 2001;74:901–904. Patlas M, Farkas A, Fisher D, et al. Ultrasound vs CT for the detection of ureteric stones in patients with renal colic.
- Crit Ultrasound J. 2013;5(Suppl 1):Vallone G, Napolitano G, Fonio P, et al. US detection of renal and ureteral calculi in patients with suspected renal colic.
- Eur Radiol. 2011;21:1535–1545.Van Randen A, Laméris W, van Es HW, et al. A comparison of the accuracy of ultrasound and computed tomography in common diagnoses causing acute abdominal pain.
- N Engl J Med. Smith-Bindman R, Aubin C, Bailitz J, et al. Ultrasonography versus computed tomography for suspected nephrolithiasis.2014;371:1100–1110.
- Radiology ; Lukasiewicz A, Bhargavan-Chatfield M, Coombs L et al (2014) Radiation dose index of renal colic protocol CT studies in the United States: a report from the American College of Radiology National Radiology Data Registry. 131601. doi:10.1148/radiol.14131601
- Abdom Imaging. 2013;38:863–869.Ripollés T, Martínez-Pérez MJ, Vizuete J, et al. Sonographic diagnosis of symptomatic ureteral calculi: usefulness of the twinkling artifact. doi: 10.1007/s00261-012-9946-7.
- J Ultrasound Med. 2012;31:1703–1711.Moore CL, Scoutt L. Sonography first for acute flank pain?
- Acad Life Emerg med: Top 10 reasons NOT to order a CT scan for suspected renal colic April 10th, 2014 | Expert Peer Reviewed (Clinical), Genitourinary, Radiology |9 Comments
By: Daniel Firestone, MD RDMS





