
Images Sarah Vaughan (Emergency Registrar) Text Genevieve Carbonatto
A young 30 year old lady is brought in by ambulance with acute onset severe lower abdominal pain. The first thing you want to exclude is a ruptured ectopic. On arrival she is pale and looks shocked. She says she had a positive pregnancy test 2 days ago but has not had a formal scan. Her BP is 85/60, her HR 90/min. On palpation suprapubically she is extremely tender. She remains in the resuscitation room on continuous monitoring, a large iv line is inserted, bloods are taken for FBC, electrolytes, BHCG, coagulation screen and blood group and hold and Xmatch. You do a FAST (focussed abdominal ultrasound) . This is her right upper quadrant scan.
This is her left upper quadrant scan.
There is clearly massive amounts of free fluid in the peritoneal cavity.
A pelvic ultrasound is then performed. This is her pelvis in long


The uterus does not show a gestational sac but there is blood within the uterus. This is a pseudosac.
By fanning slightly to the right, a corpus luteal cyst is visible.
Power Doppler can cause the appearance of a “ring of fire” around the CL cyst. This is due to peritrophoblastic blood flow. Here there is flow visible partially around the CL cyst.
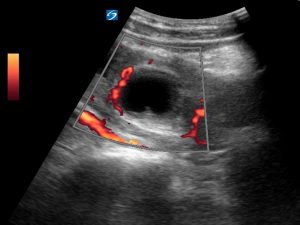
With the CL cyst in the middle of the image and fanning ever so slightly medially longitudinally, the tubal ring of the ectopic appears.
By zooming onto this tubal ring, a yolk sac and fetal pole appears. Within the centre of the fetal pole there is a heart beat confirmed by using M mode.The tubal ring has been referred to as the “bagel sign”.


Clip showing fetal heart visible in the middle of the fetal pole
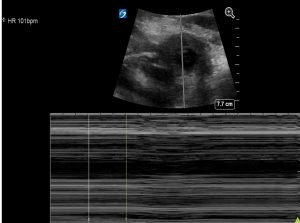
M mode showing fetal HR of 110/min
Power Doppler also causes the appearance of a “ring of fire” due to the increased vascularity around the gestational sac.

The patient is immediately transferred to theatres where the right ectopic pregnancy was removed. An estimated 2l of blood was found in her peritoneal cavity. She was transfused 2 U of blood. Her BHCG came through as 23,710 IU/L and her progesterone level as 72.9nmol/l. Her haemoglobin before theatre was 112g/l and 88g/l post surgery.
Discussion
In Australia the incidence of ectopic pregnancy decreased slightly in the 1990s, from a rate of 17.4 per 1000 births in 1990 to 16.2 per 1000 in 1998. The prevalence of ectopic pregnancy in patients who present to the Emergency Department with first trimester bleeding or pain ranges from 6 to 16%. There were 3 deaths from ectopic pregnancy in Australia between 2006 and 2010. (1). Ectopic pregnancy deaths are rare because of early diagnosis and a high level of suspicion of rupture in the emergency department if a women presents with abdominal pain +/- PV bleeding.
Sudden acute abdominal pain in early pregnancy should be considered to be due to a ruptured ectopic until proved otherwise. Intraperitoneal fluid on a FAST exam as in the case presented here almost clinches the diagnosis however the differential diagnosis of acute pain in early pregnancy like this is a ruptured CL cyst. Free abdominal fluid can also be seen with a ruptured CL cyst. In this case a ruptured ectopic with a yolk sac and fetal pole demonstrating an active heart beat was visible. Tubal vessels can rupture causing significant intraperitoneal bleeding without causing immediate fetal demise as demonstrated in this case. An empty uterine cavity is helpful in estimating the likelihood of an ectopic in this situation. Having said that an empty uterine cavity could be due to a gestational age which is too early to visualise by trans abdominal ultrasound.(4)
The most common sonographic findings in the emergency department are free fluid in the peritoneal cavity, an empty uterus and a complex adnexal mass. In this case we have massive amounts of blood in the peritoneal cavity, a uterine cavity with a pseudosac, a right sided CL cyst with an ipsilateral ectopic pregnancy which contains a live intrauterine fetus.
Ultrasound findings in ruptured ectopic pregnancy
- Intraperitoneal fluid
- Free fluid in Morison’s pouch and pouch of Douglas
- Note that haemorrhage in the pouch of Douglas is not infrequently echogenic (it has clotted) and therefore easily missed.
2. Empty uterus
- Caution should be exercised on transabdominal ultrasound if the pregnancy is very early as a gestational sac may not be visible
- A pseudosac may be present in 5 -10% of ectopic pregnancies
- A pseudosac is not a sac at all but an intrauterine fluid collection.
- It can mimic an intrauterine gestational sac
- It is generally irregularly shaped with pointed edges and/or filled with debris
- It is centrally located rather than eccentrically located
- It does not contain a yolk sac
3. Complex mass
- Most common sonographic finding in adnexa
- Indistinct mass which could be a tubal miscarriage or a tubal rupture
4. Tubal ring
- Ectopic gestational sac, most commonly seen in unruptured ectopic rather than ruptured ectopic pregancies
- “Bagel sign” hypoechoic centre (+/- yolk sac) surrounded by thick echogenic rim
- The echogenic rim is due to concentric trophoblastic tissue surrounding the chorionic sac of the ectopic pregnancy.
- Power Doppler will demonstrate peritrophoblastic flow (intense circumferential flow on colour Doppler with high velocity, low resistance Doppler signal on spectral analysis)
5. CL cyst
- CL cysts are ipsilateral to the ectopic pregnancy in 70% of cases
- Power Doppler will show a “ring of fire” surrounding the CL cyst
Teaching point: While transabdominal ultrasound is not as sensitive as transvaginal ultrasound in early pregnancy, the skill to correctly identify an intrauterine pregancy is useful in screening for early pregnancy complications. Ectopic pregnancy should be suspected when no intra uterine pregancy (IUP) is found on preliminary scanning (2).Ectopic pregnancy remains the leading cause of death in first trimester pregnancy. A meta-analysis looking at emergency physician focussed point of care pelvic ultrasonography found that it had a sensitivity of 99.3% and a negative predictive value of 99.96% in detecting an intrauterine pregnancy. Given a disease prevalence of 7.5% and a negative likelihood ratio of 0.08, visualization of an intrauterine pregnancy by an emergency physician yields a posttest probability of ectopic pregnancy of 0.6% (2), therefore visualisation of an intrauterine pregnancy by an emergency physivian is generally sufficient to rule out an ectopic pregnancy. (3)
References
- Maternal deaths in Australia 1006 -2010 Austrlian Government. Australian institute of health and welfare.
- Journ Accid Emerg Med .1998 May; 15(3): 155–158.Efficacy of transabdominal ultrasound examination in the diagnosis of early pregnancy complications in an emergency department.
T W Wong, C C Lau, A Yeung, L Lo, and C M Tai - Ann Emerg Med. 2010 Dec;56(6):674-83.Emergency physician ultrasonography for evaluating patients at risk for ectopic pregnancy: a meta-analysis. Stein JC1, Wang R, Adler N, Boscardin J, Jacoby VL, Won G, Goldstein R, Kohn MA.
- Srp Arh Celok Lek 2013 Sep-Oct;141(9-10):689-92 Ruptured corpus luteum cyst in early pregnancy: a case report. Vidaković S1, Dokić M1, Vilendecić Z1, Maravić MD1.
- CMAJ 2005 Oct 11; 173(8): 905–912. Diagnosis and treatment of ectopic pregnancy Heather Murray, Hanadi Baakdah, Trevor Bardell, and Togas Tulandi
- Radiopaedia.org





