
Ultrasound images and text Genevieve Carbonatto. Featured image: Oceanographic museum Monaco.
A 45 year old man presents to the Emergency Department with a 6-month history of feeling generally unwell with fevers and a chronic cough. He is no longer able to cope at home.
On arrival he is saturating 90% on RA (room air), his BP is 90/60, his HR 140/min (sinus rhythm). Temperature 37.8. He looks exhausted
His WCC is 20 and his CRP 260, his electrolytes are normal as are his liver and renal function.
On examination he has decreased AE (air entry) in his basal left lung field.
This is his Xray

There is a large left sided pleural effusion with mediastinal shift to the right.
A point of care ultrasound is performed which identifies the fluid more clearly
The lung can be seen clinging to the wall of the thoracic cavity un aerated, and fibrin strands can be seen floating in the fluid. The fluid is not completely anechoic, cells can be seen swirling in the fluid. This has been described by Lichtenstein as ” pea soup”.
In this clip, the unaerated lung tissue is clearly seen adjacent to the heart and within the tissue there are two abscesses visible. One anterior to the heart and one just inferior to the heart.

An empyema is therefore the most likely diagnosis. Fluid is drained from the left chest which is cloudy and foul smelling. Broad spectrum antibiotics are started (Tazocin). A CT is organised.
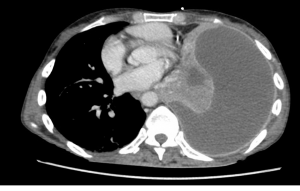
The CT demonstrates an extensive pleural effusion and also identifies pulmonary abscesses, one of which can be seen on this CT slice.
The patient is taken to theatre for a left thoracotomy and pulmonary decortication. The pleural fluid culture comes back later growing actinomyces meyeri.
Discussion
The sensitivity of ultrasound for the evaluation of pleural fluid should make it a routine test in patients who present with effusions. Ultrasound can differentiate between consolidation and pleural fluid. It is highly sensitive in identifying pleural fluid and much more sensitive than chest Xray (93% vs 47%) (1). Chest X-rays can detect fluid only if it is greater than 200mls, the sensitivity of which decreases in the supine patient, while as little as 20 mls can be detected with ultrasound (2) Ultrasound can be used to assess the quantity of pleural fluid (3) by using the “PLAPS index” as described by Lichtenstein, however generally a qualitative rather than an accurate quantitative approach is enough in clinical practice.
Ultrasound can identify septations and allows the identification of the best site for thoracocentesis. Ultrasound reduces the risk of complications such as pneumothorax with thoracocentesis.
Ultrasound can also give an idea of the nature of the pleural fluid but is not entirely reliable in doing so (3). Pleural effusion patterns in sonographic appearances can be subclassified as anechoic, complex nonseptated, complex septated and homogeneously echogenic. Anechoic effusions can be either transudates or exudates and echoic effusions are usually exudates although some transudates frequently show echogenic material (5). In short, a pleural tap under ultrasound guidance if clinically indicated can categorically differentiate between exudate and transudate.
Lung ultrasound has been shown by Lichtenstein to be highly sensitive in diagnosing pleural fluid, pneumothorax, consolidation and interstitial syndrome. CT scans have their place in the evaluation of the patient with SOB (shortness of breath) but ultrasound offers the possibility of replacing CT scans in certain clinical situations (4). CT scans can be time consuming, involve significant radiation and may be pose a risk with transportation in the critically ill (6) Ultrasound, because it enables the visualisation of moving lung, gives greater clarity than CT scans in evaluating septations and debris in pleural fluid. In our patient, lung abscesses, purulent fluid, fibrin strands and unaerated lung were much better visualised and “understood” with ultrasound.
Teaching point: Ultrasound should be used in all patients in the evaluation of SOB in the Emergency Department. The highly sensitive nature of ultrasound in the evaluation of pleural fluid and lung pathology makes it an essential imaging modality. The very nature of ultrasound, which enables the real time visualisation of the moving lung, makes this imaging modality a valuable and essential tool.
References
- Anaesthesiology 2004 Jan;100(1):9-15.
Comparative diagnostic performances of auscultation, chest radiography, and lung ultrasonography in acute respiratory distress syndrome.
Lichtenstein D1, Goldstein I, Mourgeon E, Cluzel P, Grenier P, Rouby JJ. - Acad. Radiol. 1996 Feb;3(2):103-9.
Pleural fluid volume estimation: a chest radiograph prediction rule.
Blackmore CC1, Black WC, Dallas RV, Crow HC. - Whole Body Sonograghy in the critically ill: Daniel Lichtenstein, Springer
- Réanimation 12 (2003) 19–29 Daniel Lichtenstein
- Ultrasound. Med.Biol 2008 Mar;34(3):362-9. Epub 2007 Nov 8.
Sonographic appearances in transudative pleural effusions: not always an anechoic pattern.
Chen HJ1, Tu CY, Ling SJ, Chen W, Chiu KL, Hsia TC, Shih CM, Hsu WH - Ann. Thorac Med. 2014 Oct-Dec; 9(4): 185–186.
Thoracic ultrasound: Picture worth a thousand sounds
Ajit Moghekar and Atul Mehta





