Question 1
The “classic” presentation of a ruptured AAA is the triad of abdominal back or flank pain , a palpable abdominal aorta and hypotension. What percentage of patients present with this triad?
Less than 25% of patients present with this presentation which is why a high clinical suspicion of a ruptured AAA and the ability to ultrasound the aorta in the ED is so important.
Question 2
- Where are the vast majority of abdominal aneurysms found?
- Name 2 shapes of aortic aneurysms.
The vast majority of aneurysms are infrarenal > 95%
a.  b.
b. 
a. infrarenal b. suprarenal
The vast majority of abdominal aneurysms are fusiform > 90% , but sometimes they may be saccular and present as a small outpouching from the aorta. Saccular aneurysms may be missed if the aorta is not carefully scanned from it’s proximal portion to it’s bifurcation.
a.  b.
b.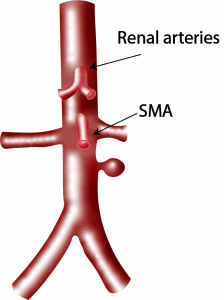
a. 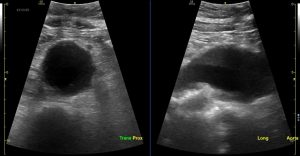 b.
b. 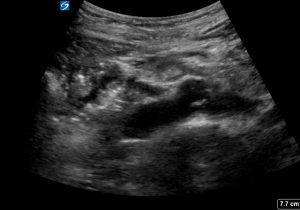
a. fusiform aneurysm in the transverse and longitudinal plane b. saccular aneurysm in the longitudinal plane
3. Most patients who present to the Emergency Department are not fasted . What are some techniques that can be used to help identify the aorta in the patient who presents to the Emergency Department
Obesity, bowel gas and bowel content may obscure the view of the aorta
- Try graded compression
- Use your left hand to put pressure on the abdomen and put the probe between the fingers of the left hand to displace as much gas as possible
- Get the patient to breath in. It may bring down the liver
- Sit the patient up.
- Get the patient to lie on their left side and look in the right axillary line through the liver and kidney
- Get the patient to roll onto their right side and look through the spleen and kidney
4. Name 6 ways you can differentiate between the IVC and the aorta when scanning the aorta.
- The IVC lies to the right of the aorta.
- It is thin walled
- It does not have calcification of it’s walls.
- It collapses with inspiration.
- It has no anterior branches
- With PW doppler you see a continuous wave form rather than a pulsatile one
Note that both IVC and aorta can be pulsatile




